Wound healing, hemostasis phase and inflammatory phase
Hemostasis phase
The hemostasis phase is the immediate response to injury to prevent blood loss at the wound site in the first few minutes. Damage of capillaries and bleeding triggers a cascade of vasoconstriction and coagulation through extrinsic and intrinsic pathways, leading to platelet aggregation and formation of blood clot consisting of fibrin and fibronectin, which plugs the wound. Platelets also release cytokines, chemokines and growth factors, including PDGF, VEGF and TGF-β, which promote the recruitment and migration of inflammatory cells (neutrophils and macrophages) as well as fibroblasts and endothelial cells to the site of injury.
Infllammatory phase
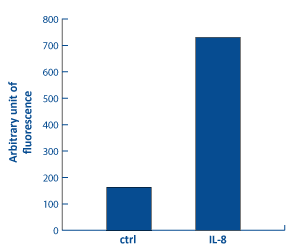
The inflammatory phase is characterized by the sequential infiltration of polymorphonuclear neutrophils (PMNs), monocytes/macrophages and lymphocytes. IL-8 facilitates PMNs migration from surrounding blood vessels [Bioassay: PMN-0009]. By phagocytozing infectious invaders and cellular debris and secreting proteases (matrix metalloproteinases and elastase), PMNs cleanse the wound. They also generate reactive oxygen species [Bioassay: PMN-0005], and together with keratinocytes, release antimicrobial and cytotoxic peptides (AMPs), like β-defensins, RNAse 7, S100A7, and LL-37, thus contributing to host defence [Bioassays: NHEK-00035 ; NHEK-0037 ; EPIBA-0050].
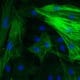
Analysis of PMN migration by
fluorescence based assay
[Bioassay: PMN-0009]
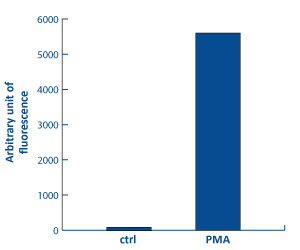
Analysis of H2O2 content in PMN by
fluorescence based assay
[Bioassay: PMN-0005]
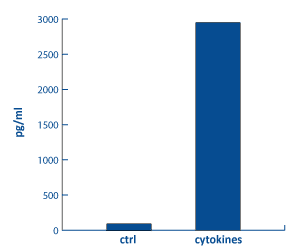
Analysis of β-défensin 2 in
epidermal keratinocytes by ELISA
[Bioassay: NHEK-0035]
Meanwhile, monocytes, attracted by chemotactic agents including TGF-β, PDGF, elastin and collagen breakdown products, migrate into the wound and differentiate into mature macrophages. Macrophages continue the cleansing process, fight infections and produce tissue growth factors (FGF, EGF, TGF-β…) as well as inflammatory (TNF-α, IL1-β, IL-8 and IL-6) and anti-inflammatory cytokine (IL-10), which activate keratinocytes, fibroblasts and endothelial cells involved in the next step of repair. More specifically, TGF-βs have a pivotal role in scar formation by acting on cell targets via SMAD and Wnt-dependent pathways, with scarring or anti-scarring effects depending on the TGF-β isoform . Lymphocytes T lastly enter the site >36h after injury.
Check out Bioalternatives’ updates and experience new testing ideas
- Bioassays, models and services
- Posts and publications
- Events



Wound healing, granulation phase and maturation phase
Wound healingThe third phase of wound healing, consisting in the replacement of the provisional fibrin matrix with granulation tissue once the wound has been debrided, includes several sub-phases: re-epithelialization, fibroplasia, collagen deposition and angiogenesis.
Wound healing, hemostasis phase and inflammatory phase
Wound healingThe inflammatory phase is characterized by the sequential infiltration of polymorphonuclear neutrophils (PMNs), monocytes/macrophages and lymphocytes. IL-8 facilitates PMNs migration from surrounding blood vessels.
Wound healing, overview
Wound healingWound healing is a complex and dynamic process of restoring skin cellular structures and tissue layers that involves multiple components: differentiated cells , stem cells , hair follicles, extracellular matrix (ECM) proteins, cytokines networks, microRNAs , blood vessels, nerves and mechanical forces.
Study of proliferation and 3D epidermal reconstruction from foreskin, auricular and trunk keratinocytes in children
Wound healingOur studies highlight the potential of foreskin tissue for autograft applications in boys. A suitable alternative donor site for autologous cell transplantation in female paediatric burn patients remains an open question in our department. We tested the hypothesis that in vitro studies and RHE reconstructive capacities of cells from different body sites can be helpful to select an optimal site for keratinocyte isolation before considering graft protocols for girls.
Epidermal healing in burns: autologous keratinocyte transplantation as a standard procedure: update and perspective
Wound healingIn the contexte of skin graft, cell suspensions transplanted directly to the wound is an attractive process, removing the need for attachment to a membrane before transfer and avoiding one potential source of inefficiency. Choosing an optimal donor site containing cells with high proliferative capacity is essential for graft success in burns.
Foreskin-isolated keratinocytes provide successful extemporaneous autologous paediatric skin grafts
Wound healingWe report a successful method for grafting paediatric males presenting large severe burns through direct spreading of autologous foreskin keratinocytes. This alternative method is easy to implement, improves the quality of skin and minimizes associated donor site morbidity. in vitro studies have highlighted the potential of foreskin tissue for graft applications and could help in tissue selection with the prospect of grafting burns for girls.
Quantitative and qualitative study in keratinocytes from foreskin in children: Perspective application in paediatric burns
Wound healingKeratinocytes from foreskin have a high capacity for division. A potential source of cells to provide coverage in paediatric burns.
Human embryonic stem-cell derivatives for full reconstruction of the pluristratified epidermis: a preclinical study
Cell and tissue engineering, Dermatology, Pharmacology, Wound healingTo assess whether the keratinocyte progeny of human embryonic stem cells (hESCs) could be used to form a temporary skin substitute for use in patients awaiting autologous grafts, we investigated the cells’ capability of constructing a pluristratified epidermis.
Cultured keratinocyte cells from foreskin and future application for burns in children
Wound healingThe keratinocytes resulting from foreskin have a high capacity of division. These cells can divide a long time before differentiation. The observations enable us to propose with our patients the keratinocytes from foreskin for wound healing especially for burns in children.
Stimulation of the proliferation of human dermal fibroblasts in vitro by a lipidocolloid dressing
Wound healingThe effect of Urgotul on normal human dermal fibroblast proliferation was studied in vitro and compared with that of two other dressing: Mepitel and Tulle Gras.